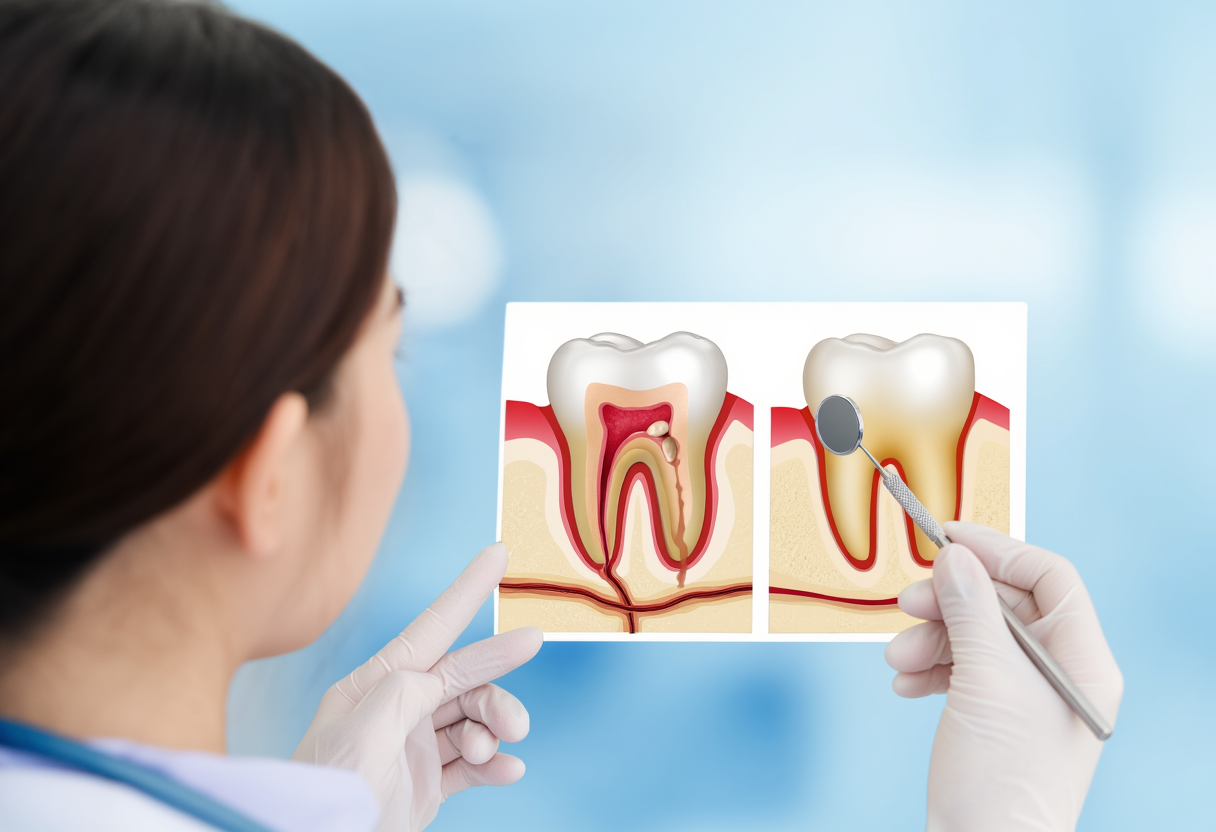
The Difference Between Gingivitis and Periodontitis
Discover the key distinctions between gingivitis and periodontitis, two common gum diseases that affect your overall oral health. Gingivitis, the early reversible stage marked by inflammation and bleeding, contrasts sharply with periodontitis, which causes irreversible bone loss and tooth damage. Learn about symptoms, risk factors like poor hygiene and smoking, essential diagnosis methods, and effective treatment options to prevent long-term complications. By prioritizing prevention through daily care and regular dental visits, you can safeguard your smile and avoid serious issues like tooth loss. Empower yourself with knowledge to maintain healthy gums for life.
The Difference Between Gingivitis and Periodontitis
Introduction to Oral Health Basics
Understanding oral health basics is essential for maintaining a vibrant smile and overall wellness. Healthy gums act as the foundation for strong teeth, serving as a protective barrier that anchors teeth securely in place and shields them from harmful bacteria and daily wear. However, plaque buildup—a sticky film of bacteria—can quickly trigger inflammation if not addressed early, leading to gum disease that starts with mild irritation but may escalate to significant damage. This progression can affect not just your mouth but also your confidence, causing persistent bad breath, discomfort while chewing, and even tooth loss over time. By focusing on oral health basics, you can prevent these issues and enjoy a healthier life.
What is Gingivitis?
Gingivitis represents the earliest and most common stage of gum disease, characterized by reversible inflammation caused primarily by plaque accumulation. Simply put, it occurs when bacteria irritate the gum tissue due to everyday habits like inadequate brushing, skipping flossing, or allowing tartar to form. Common symptoms include red, swollen gums that bleed easily during brushing or flossing, signaling the need for immediate attention. The good news is that with prompt care, such as improved oral hygiene routines, gingivitis can typically be reversed before it causes lasting harm. Regular dental checkups are crucial to catch this early stage and prevent progression.
What is Periodontitis?
Periodontitis marks an advanced and more severe form of gum disease where the infection extends beyond the gums to affect the connective tissues and jawbone. This condition often develops from untreated gingivitis, as bacteria deepen their invasion and create pockets between the gums and teeth that harbor more plaque. Symptoms escalate to include gum recession, noticeable bone loss, persistent bad breath, loose teeth, and pain when chewing. While periodontitis can be managed through professional treatments, it's not fully reversible once the supporting structures are damaged, highlighting the critical need for early intervention to avoid complications like tooth loss.
Key Differences Between Gingivitis and Periodontitis
When comparing gingivitis and periodontitis, the key differences lie in severity, symptoms, and long-term outcomes. Gingivitis involves only inflammation of the gums, whereas periodontitis includes destruction of tissues and bone, leading to more profound issues like tooth mobility and recession. Mild symptoms such as occasional bleeding contrast sharply with advanced signs in periodontitis, such as loose teeth or visible gaps. This difference underscores a higher risk of tooth loss and greater treatment complexity with periodontitis, making early diagnosis through regular dental visits essential for better, simpler outcomes. Recognizing these distinctions helps you act quickly to preserve your oral health.
Risk Factors for Gum Disease
- Poor Oral Hygiene: Inconsistent brushing and flossing allow plaque to accumulate, increasing the risk of inflammation.
- Smoking and Vaping: These habits exacerbate gum inflammation and slow healing.
- Health Conditions: Diabetes, hormonal changes (e.g., during pregnancy), and dry mouth can heighten susceptibility.
- Genetic Predispositions: Some individuals experience rapid progression due to family history.
- Lifestyle Factors: High stress, sugary diets, and certain medications also contribute to gum disease development.
Diagnosis of Gum Disease
Dentists diagnose gingivitis and periodontitis through a comprehensive evaluation that goes beyond self-assessment, as symptoms can be subtle or misleading. During a checkup, they perform visual exams to check for redness, swelling, bleeding, and plaque levels, followed by periodontal probing to measure pocket depths—a key indicator of disease severity. Dental X-rays are crucial for detecting hidden bone loss in periodontitis cases. If you notice persistent symptoms like bleeding gums or bad breath, it's wise to schedule a dental visit promptly to catch issues early. This proactive approach ensures accurate diagnosis and timely treatment.
Treatment Options
- For Gingivitis: Simple home care like enhanced brushing and flossing techniques combined with routine professional cleanings can reverse the condition.
- For Periodontitis: Deeper interventions such as scaling and root planing (a deep cleaning procedure) are common, along with antimicrobial rinses or antibiotics to combat infection.
- Severe Cases: Periodontal surgery may be necessary to restore damaged tissues and prevent further bone loss.
- Maintenance: Committing to regular dental visits is essential to prevent relapse and ensure long-term gum health.
Prevention Strategies
- Daily Oral Care: Brush twice daily with fluoride toothpaste using proper circular motions to remove plaque effectively.
- Flossing and Interdental Cleaners: Use these every day to remove plaque between teeth where brushes can't reach.
- Diet and Lifestyle: Limit sugary snacks, stay hydrated, and avoid tobacco to reduce risks.
- Regular Dental Visits: Schedule checkups and professional cleanings for early detection and sustained prevention.
- Holistic Approach: Combine these habits with stress management to empower a healthy, confident smile for life.